
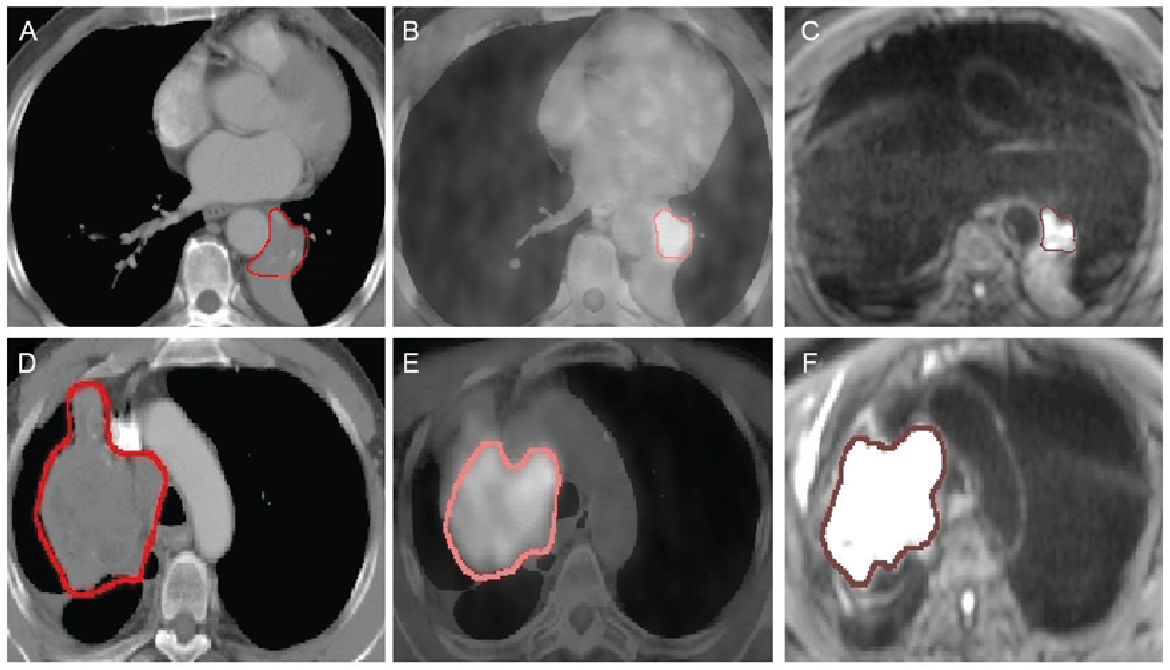
Imaging methods such as ultrasound, computed tomography (CT), magnetic resonance imaging (MRI) or positron emission tomography (PET) play an important role in diagnosis and staging, as well as vital in radiotherapy planning.
Since radiotherapy is used locally in treatment, tumor volume is determined with these imaging and plans are made to protect healthy tissues appropriately. The least complication rate is considered the basis of successful treatment.
Classically, cross-sectional imaging is used in treatment planning in radiotherapy. Subsequent treatment fractions of the patient are determined accordingly, and daily treatment adjustments are reconstructed by markings on the skin or on assistive devices such as masks. These are checked with 2D X-ray or digital imaging, and patients are treated. Positional deviations of a few millimeters may occur during treatment. Considering this possibility at the planning stage, it is tried to ensure that the target volume is reliably covered during the treatment by selecting the appropriate safety margins.
Image-guided radiotherapy (IGRT) has been integrated directly into the linear accelerator device to eliminate these drawbacks. By directly integrating imaging into the linear accelerator, patient position, possible change of tumor during treatment and possible changes in patient anatomy can be monitored daily. It enables immediate intervention in the changes that may occur according to the imaging findings during the planning phase. Treatment plans are arranged according to this new situation.