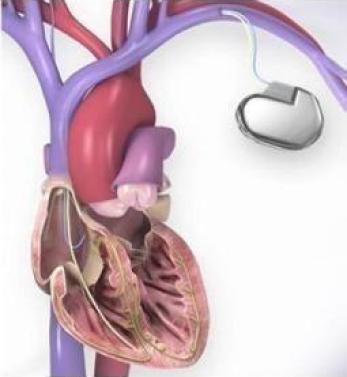
How does the ICD work?
An ICD is inserted under the skin, usually in the space just below the collarbone (clavicle), to monitor your heart rate. Thin wires connect the ICD to the heart, where it always controls your heart rate and rhythm. It monitors your heart rhythm through electrodes.
If an ICD detects a dangerous heart rhythm, they may administer one or more of the following treatments:
Pacing – a series of low-voltage electrical pulses (pulse rate) at a fast rate to try and correct the heart rhythm.
Cardioversion - one or more small electrical shocks to return the heart to its normal rhythm.
Defibrillation - one or more large electrical shocks to try to return the heart to its normal rhythm.
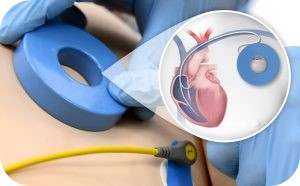
How is an ICD fitted?
ICDs are inserted under local anaesthetic but with sedation, so you'll feel very sleepy. It can take anything from one hour to three or more hours to implant an ICD. The time it takes will depend on the type of device you are given. You'll often (but not always) need to stay overnight in hospital and your ICD will be thoroughly checked before you leave.
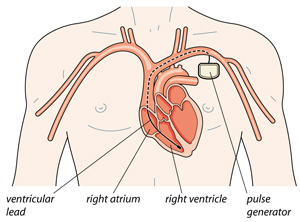
The ICD is inserted just under your collar bone. It looks similar to a pacemaker and is a little bigger than a matchbox.
An ICD is made up of:
a pulse generator – a battery powered electronic circuit
one or more electrode leads, which are placed into your heart through a vein.
A different type of ICD is suitable for some people. It's called a subcutaneous (under the skin) ICD – or SICD for short. An SICD works in the same way as an ICD, but it's inserted under the skin of the chest (outside of the ribcage) and there are no leads placed into the heart. Your doctor will talk to you about this option if it's right for you.
Who needs an ICD?
You might need an ICD if:
you have already had a life-threatening abnormal heart rhythm and are at risk of having it again
you haven't had a life-threatening heart rhythm, but tests show you are at risk of one in the future. This is usually because you have inherited faulty genes and may have a condition such as Cardiomyopathy, Long QT syndrome or Brugada syndrome
you have heart failure and are at risk of developing a life-threatening heart rhythm. This is called cardiac resynchronisation therapy with a defibrillator, or CRT-D. This single device combines a pacemaker with an ICD. The leads and the CRT-D work together to make sure that the ventricles beat in time.
How do I live with an ICD?
It's important to have regular follow-up appointments at your ICD clinic, so you can have your ICD checked. Your appointments may be every 3 to 12 months, depending on the type of ICD you have and if it has delivered any treatment. You'll need to have follow-up appointments for the rest of your life.
Some ICD checks may be done remotely with the information from your ICD sent via a signal on the device or a home docking station to your health care professional, so there is sometimes no need to attend hospital.
You may have to make some changes to your lifestyle, for instance, if you drive or take part in contact sports. You also need to be aware of how some electronic devices, such as TENS machines or airport security systems, can affect your ICD.
Your doctor will discuss this with you, and you can find out more in our.
Will my mobile phone affect my ICD?
It's ok to have a smartphone when you have an ICD, though care should be taken in case they contain magnetic material. It's recommended that smartphones are kept at least 6 inches away from where your device is.
Apple iPhone 12 models, including other products like iPads, contain extra magnets in their charging functions that could turn off ICDs. Apple advise that you keep these products and their charging accessories more than 6 inches away from your device, or more 12 inches away if charging wirelessly (when the magnets are in use).
Don't worry too much if your phone gets too close to your ICD, as they're designed to return to their normal settings once the magnet is moved away.
If you're unsure about your phone for any reason, we recommend you check its handbook/instructions or talk to the manufacturer. You could also contact your doctor or pacing clinic if you have concerns about your device.
Who can I talk to about my ICD?
It's natural to feel worried about having an ICD fitted and it often helps to talk about your feelings with someone close to you or with a healthcare professional.